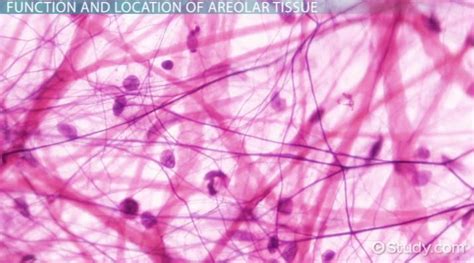
Areolar Connective Tissue: A Practical Guide to Understanding Its Key Locations
Areolar connective tissue is a versatile type of tissue found throughout the body. Understanding where and how it functions can help in various medical fields, from pathology to surgery. This guide aims to provide step-by-step guidance with actionable advice on discovering areolar connective tissue's key locations, making it accessible and practical for everyone from medical students to healthcare professionals.
Understanding the Need for Identifying Areolar Connective Tissue
Identifying areolar connective tissue is essential for diagnosing and understanding a variety of conditions. It plays a critical role in holding organs in place, maintaining the shape of structures like lymph nodes and mucous membranes, and serving as a reservoir for nutrients and water. Misidentifying or overlooking this tissue can lead to incorrect diagnoses and inadequate treatment plans. Therefore, knowing its key locations is crucial for accurate medical assessment and treatment.
Quick Reference
Quick Reference
- Immediate action item: Examine the spaces between organs and structures to locate areolar connective tissue.
- Essential tip: Use a microscope for a detailed examination of cellular composition, focusing on fibroblasts, collagen fibers, and adipocytes.
- Common mistake to avoid: Confusing areolar tissue with dense connective tissue; remember areolar tissue is less organized with more ground substance.
Detailed Exploration of Areolar Connective Tissue Locations
Areolar connective tissue is often overlooked but is integral to various bodily functions. Let’s dive into its key locations, providing practical examples and detailed how-to sections for proper identification.
Under the Skin: Subcutaneous Layer
Areolar connective tissue exists just beneath the skin, forming the subcutaneous layer. This layer serves as a cushion, providing insulation and protection from mechanical injuries.
To identify this tissue:
- Visual Inspection: Look at areas where skin is stretched, such as the abdomen or thighs. The loose skin indicates the presence of areolar tissue.
- Palpation: Gently press the skin over the area; you’ll feel the layer of fat and connective tissue separating the skin from underlying muscles.
This layer’s role is critical in maintaining skin elasticity and flexibility.
Around Organs: Omentum and Mesentery
Areolar connective tissue forms the omentum, which hangs down from the stomach, and the mesentery, which attaches the intestines to the abdominal wall.
To examine these areas:
- Visual Identification: In surgical procedures, observe the omentum’s loose connective tissue wrapping around abdominal organs.
- Palpation: Feel the mesentery during surgical exploration; it feels slippery and holds intestines loosely.
These structures are vital in holding and protecting abdominal organs.
Beneath Mucous Membranes: Respiratory and Digestive Tracts
Areolar tissue is found beneath mucous membranes lining the respiratory and digestive tracts. This layer ensures smooth movement and support for internal organs.
To explore these areas:
- Visual Identification: During endoscopy, notice the thin layer beneath the mucous membrane in the respiratory or digestive tract.
- Histological Examination: Use a microscope to observe cellular components such as fibroblasts and collagen fibers.
This tissue’s role is to provide support while allowing flexibility for organ movement.
Supporting Structures: Lymphatic System
Areolar connective tissue supports the structure of lymph nodes and other lymphatic organs. It holds cells together and provides a framework for immune cell circulation.
To locate and study this tissue:
- Visual Identification: During lymph node biopsies, observe the soft, fibrous tissue holding nodes together.
- Histological Examination: Look at tissue samples under a microscope to identify fibroblasts, collagen, and other fibers.
This tissue’s role is critical for immune system function and lymph circulation.
Under Muscles: Fascia and Epimysium
Areolar connective tissue forms layers of fascia around muscles and the epimysium that covers individual muscles. It allows muscles to move freely and provides structural support.
To identify areolar tissue in these areas:
- Visual Identification: During dissection, observe the fascia that envelops muscles and the epimysium covering muscle tissue.
- Palpation: Feel the fascia’s thin, fibrous layer during surgical or physical examination.
This tissue is essential for muscle flexibility and support.
Practical FAQ
What makes areolar connective tissue different from other types of connective tissue?
Areolar connective tissue differs from dense connective tissue in its less organized structure and higher ground substance content. While dense connective tissue has tightly packed collagen fibers, areolar tissue has more fibroblasts, collagen fibers, and elastic fibers, making it less dense but more flexible. This flexibility allows areolar tissue to fill spaces and bind different tissue layers together.
Why is it important to differentiate areolar connective tissue in medical practice?
Differentiating areolar connective tissue is crucial for accurate diagnosis and treatment. Misidentifying it can lead to incorrect assessments, such as confusing it with more rigid types of connective tissue during surgeries or biopsies. Understanding its unique properties and locations helps in procedures like organ repair, tumor removal, and inflammatory disease management.
Conclusion
Areolar connective tissue is a fundamental component of the body’s structure and function. By identifying its key locations—under the skin, around organs, beneath mucous membranes, in the lymphatic system, and under muscles—medical professionals can better understand and manage a range of conditions. This guide provides practical, actionable steps to ensure you can confidently recognize areolar connective tissue in various contexts. Applying these insights can significantly improve medical practice, from diagnosis to treatment planning, ensuring more accurate and effective healthcare outcomes.