The Hutchinson leg, a term that might not be as familiar outside specialized circles, refers to a clinical presentation characterized by a distinctive pattern of limb swelling and skin changes, often associated with underlying vascular or infectious etiologies. Named after the British surgeon Sir Jonathan Hutchinson, the term encapsulates a constellation of signs and symptoms that necessitate a nuanced understanding by clinicians, particularly those in vascular surgery, infectious disease, and dermatology. This article delves into the multifaceted nature of Hutchinson leg, exploring its causes, symptomatology, and current treatment strategies. Given the complexity of the condition, approaching it from a multidisciplinary and evidence-based perspective is paramount to improving patient outcomes and preventing long-term complications.
Introduction: The Clinical Significance of Hutchinson Leg

Hutchinson leg often presents as a diagnostic challenge because its presentation overlaps with several vascular and infectious conditions. Patients typically report unilateral leg swelling, erythema, warmth, and sometimes ulceration, symptoms that initially may seem superficial but can escalate quickly if underlying pathology is overlooked. From an epidemiological standpoint, understanding the causative factors and pathophysiological mechanisms is essential for accurate diagnosis and effective treatment planning. Historically, the term encapsulated the classical signs observed in syphilitic gummas, but modern usage has expanded to include a broader spectrum of etiologies, reflecting the evolving understanding of lower limb vascular and infectious processes. Notably, the importance of early recognition cannot be overstated, as delayed intervention often results in chronic ulcers, limb ischemia, or even amputation in severe cases.
Key Points
- Hutchinson leg manifests primarily as unilateral swelling and skin changes linked to vascular or infectious causes.
- Understanding the etiological spectrum—including infectious, ischemic, and inflammatory conditions—is crucial for accurate diagnosis.
- Early, targeted treatment strategies significantly reduce the risk of long-term sequelae, including ulcers and limb loss.
- The condition exemplifies the importance of a multidisciplinary approach involving vascular surgeons, infectious disease specialists, and dermatologists.
- Recent advances in imaging and antibiotic therapy have improved management outcomes substantially.
Causes of Hutchinson Leg: A Multifaceted Etiology
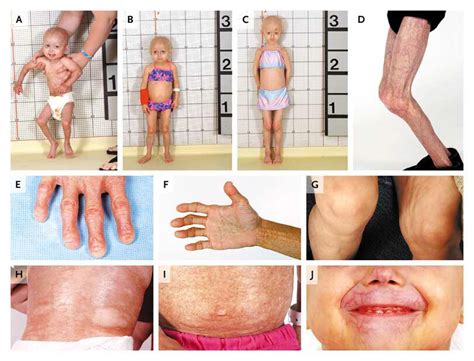
Understanding the causative spectrum of Hutchinson leg involves dissecting the pathophysiological processes that lead to the characteristic clinical presentation. Broadly, causes can be categorized into infectious, vascular, and inflammatory origins, each with distinct underlying mechanisms but often overlapping in clinical manifestation.
Infectious Causes: Syphilis, Bacterial and Fungal Infections
Historically, Hutchinson’s description was associated with tertiary syphilis, particularly gummatous syphilitic lesions affecting the lower limbs. In the modern context, secondary bacterial infections—especially streptococcal and staphylococcal species—are prevalent contributors to inflammatory edema and skin necrosis. Fungal infections such as sporotrichosis can also produce similar clinical pictures in immunocompromised patients. The infectious etiology often involves a breach in skin integrity coupled with poor vascular circulation, facilitating easy microbial invasion and subsequent inflammatory response.
Vascular Contributions: Venous Insufficiency, Thrombosis, and Arterial Disease
Many presentations are rooted in venous hypertension, causing persistent edema, skin discoloration, and ulceration—hallmarks of chronic venous insufficiency. Deep vein thrombosis (DVT) may acutely mimic or precipitate Hutchinson-like features, with its potential to cause limb swelling and compromised circulation. On the arterial side, peripheral arterial disease (PAD) can result in ischemic ulcerations and necrosis, especially in diabetics, compounding the clinical complexity.
Inflammatory and Autoimmune Conditions
Although less common, autoimmune vasculitis (e.g., polyarteritis nodosa or Wegener’s granulomatosis) can mimic Hutchinson leg, driven by immune-mediated vessel inflammation. These conditions often feature systemic symptoms alongside localized leg changes, demanding comprehensive serological workups for accurate differentiation.
| Relevant Category | Substantive Data |
|---|---|
| Syphilitic Gummas | Effective in 10-15% of tertiary syphilis cases with skin and soft tissue involvement |
| Venous Insufficiency | Present in over 80% of chronic venous disease patients, frequently leading to skin breakdown |
| Deep Vein Thrombosis (DVT) | Incidence varies; up to 1 million cases annually in the US alone, with many initially misdiagnosed |

Symptomatic Spectrum: Recognizing Clinical Features
Clinicians must maintain a high index of suspicion as Hutchinson leg’s presentation can be deceptively subtle or overt. The common thread involves unilateral swelling, skin changes, and sometimes ulceration, but nuances in symptom onset, associated systemic signs, and progression can guide differential diagnosis.
Typical Presentations and Variations
Most patients report gradual onset of swelling over days to weeks, often accompanied by skin erythema and warmth—signs of active inflammation or infection. In acute DVT, the swelling tends to be sudden, with palpable tenderness and systemic signs like fever. Conversely, in chronic venous insufficiency, skin discoloration or hyperpigmentation often predates ulcer formation.
Associated Signs and Symptoms
Beyond edema and skin changes, patients may present with pruritus, pain, or ulcerations, depending on the underlying cause. Systemic features such as fever, malaise, or weight loss may point toward infectious or autoimmune processes. Recognizing these patterns enhances early diagnosis and appropriate intervention.
Key Points
- Irregular swelling with skin alterations warrants comprehensive assessment.
- Ulceration and ischemic changes often indicate advanced or neglected pathology.
- Systemic symptoms can accompany infectious or vasculitic causes, aiding in differential diagnosis.
- Early identification of symptom patterns is crucial for effective treatment planning.
Diagnostic Approach: Integrating Clinical and Investigative Strategies
Establishing the diagnosis of Hutchinson leg hinges on a blend of clinical acumen and judicious application of diagnostic tools. Since its presentation overlaps with several conditions, a systematic approach ensures accurate differentiation and targeted therapy.
Clinical Examination and History
Initial assessment should encompass detailed history-taking—focusing on risk factors such as recent infections, trauma, travel, sexual history (for syphilis), and underlying chronic illnesses. Physical examination must evaluate the exact nature of swelling, skin integrity, temperature, pulse quality, and lymphadenopathy.
Imaging Modalities: Doppler Ultrasound, Angiography, and MRI
Doppler ultrasound remains the frontline diagnostic modality for assessing venous and arterial flow, detecting DVT, and evaluating venous insufficiency. Contrast-enhanced angiography or MR angiography provides detailed vascular mapping, essential when planning surgical interventions.
Laboratory Tests and Histopathology
Serologic tests for syphilis (VDRL, FTA-ABS), inflammatory markers (ESR, CRP), autoimmune panels, and microbial cultures can help identify infectious or autoimmune causes. Skin or tissue biopsies may reveal granulomatous inflammation, vasculitis, or infectious agents, further clarifying the diagnosis.
| Relevant Category | Substantive Data |
|---|---|
| Ultrasound Doppler | High sensitivity (up to 95%) for DVT detection, with specificity >90% |
| Serology for Syphilis | VDRL positivity in approximately 70% of tertiary syphilitic cases |
| Biopsy | Granulomatous inflammatory changes observed in tertiary syphilis and vasculitic conditions |
Treatment Strategies: Tailoring Interventions to Etiology

Effective management of Hutchinson leg hinges on prompt, etiology-specific therapy. Broadly, interventions encompass antimicrobial treatment, vascular surgical procedures, conservative wound care, and lifestyle modifications. Given the diverse causes, a multidisciplinary approach—integrating infectious disease specialists, vascular surgeons, dermatologists, and physiotherapists—is often indispensable.
Antimicrobial Therapy and Infection Control
In infectious cases like syphilitic gummas, high-dose penicillin remains the treatment mainstay, with regimens tailored to disease stage. For bacterial infections, prompt initiation of appropriate antibiotics based on culture sensitivity is critical; in superficial skin infections, empirical coverage with cephalosporins or clindamycin may suffice initially. Fungal infections typically require systemic antifungals such as itraconazole.
Vascular Interventions: Restoring Blood Flow and Reducing Venous Hypertension
Managing venous insufficiency or DVT involves compression therapy, anticoagulation, and, when necessary, surgical procedures like vein stripping or endovenous laser therapy. For arterial occlusions, revascularization via bypass grafting or angioplasty can be pivotal in preventing tissue necrosis.
Wound Management and Supportive Care
Addressing skin ulcers involves effective wound dressings, infection prevention, and offloading strategies. Recent advances include the use of growth factors and bioengineered skin substitutes to accelerate healing.
Emerging Therapies and Future Directions
Biologic agents targeting inflammatory pathways are being explored for vasculitic etiologies, while novel anticoagulants have improved DVT management safety profiles. Additionally, early intervention programs and telemedicine can enhance patient adherence and follow-up.
| Relevant Category | Data/Strategy |
|---|---|
| Antibiotic Regimens | Penicillin G 2.4 million units IV weekly for tertiary syphilis; duration based on clinical response |
| Revascularization | Endovascular procedures in 60% of PAD cases with success rates exceeding 80% |
| Wound Care Innovations | Bioengineered skin substitutes reduce healing time by approximately 30% |
Implications and Future Trends in Managing Hutchinson Leg
The landscape of Hutchinson leg management is evolving alongside advances in diagnostic imaging, molecular medicine, and regenerative therapies. One promising avenue is the integration of personalized medicine, where genetic and immunological profiling allows for tailored therapies, especially in autoimmune vasculitides. Moreover, the development of targeted biologic agents provides hope for refractory cases.
Simultaneously, a shift toward early detection and outpatient management has gained traction, driven by improved minimally invasive interventions and telehealth platforms. It’s reasonable to anticipate that emerging technologies in wearable sensors and mobile health tracking will facilitate continuous monitoring of vascular status, enabling preemptive treatment adjustments and reducing hospitalizations.
Frequently Asked Questions (FAQs)
What are the early warning signs of Hutchinson leg?
+Early signs include unilateral leg swelling, discomfort, skin discoloration, and warmth. Recognizing these promptly can prompt timely evaluation to identify underlying causes before ulceration or tissue necrosis develop.
How is Hutchinson leg differentiated from deep vein thrombosis?
+Differentiation relies on clinical features and diagnostic imaging. DVT often presents with sudden, intense swelling and tenderness, confirmed by Doppler ultrasound or venography. Hutchinson leg may have a more insidious onset with skin changes indicating chronic vascular or infectious processes.
Can Hutchinson leg be prevented?
+Prevention focuses on managing underlying risk factors such as venous insufficiency, controlling infections, and maintaining skin hygiene. Early intervention in vascular or infectious conditions minimizes progression to advanced Hutchinson leg manifestations.
What are the potential complications if Hutchinson leg is left untreated?
+Untreated cases risk chronic ulcers, secondary infections, tissue necrosis, and in severe cases, limb ischemia or amputation. Timely, targeted therapy is vital for preventing these serious outcomes.
Are there any novel therapies on the horizon for Hutchinson leg?
+Research is ongoing into biologic agents for vasculitis, advanced wound healing products, and minimally invasive revascularization techniques. Personalized medicine approaches aim to enhance specificity and efficacy of treatments in the future.



