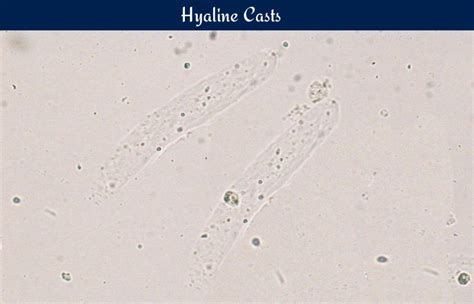
Understanding the formation and significance of hyaline casts in urine is essential for diagnosing renal health accurately. Hyaline casts, which are formed from proteinaceous material, are one of the most common types of casts found in urine. They appear as smooth, translucent cylindrical structures, and their presence can indicate underlying kidney issues. This article delves into what hyaline casts signify, their formation process, and the broader implications for medical diagnostics.
Key Insights
- Primary insight with practical relevance: Hyaline casts can indicate early-stage renal problems and overall health surveillance.
- Technical consideration with clear application: Distinguishing hyaline casts from other types of casts can inform the clinical management of renal health.
- Actionable recommendation: Routine urinalysis should include microscopic examination for casts to monitor kidney function.
Formation of Hyaline Casts
Hyaline casts form within the nephrons of the kidney, specifically in the distal tubules and collecting ducts. These casts are primarily composed of proteinaceous material derived from plasma proteins that filter into the renal tubules. Under normal conditions, the kidneys reabsorb most proteins back into circulation, but when renal filtration is impaired, these proteins aggregate and form casts. The casts then move through the urine, providing valuable diagnostic information.The formation of hyaline casts can be triggered by various conditions, such as dehydration, high protein diets, or early-stage renal pathologies. Understanding these triggers is critical for clinicians. For instance, mild exercise can temporarily increase the amount of protein in the urine, resulting in hyaline casts, particularly in young, healthy individuals. This knowledge helps in differentiating transient from persistent pathological conditions.
Clinical Significance of Hyaline Casts
Hyaline casts are typically seen in small quantities in healthy urine samples. However, an increase in their number is often indicative of renal stress or dysfunction. While hyaline casts themselves are not a direct marker of severe kidney disease, their presence is a red flag that warrants further investigation. Their detection in urine samples can lead to deeper diagnostic tests such as serum creatinine levels, glomerular filtration rate (GFR), and other renal function tests to assess the extent of renal impairment.Moreover, hyaline casts are particularly useful in distinguishing between different types of renal pathologies. For instance, their presence without accompanying red blood cells (RBCs) and white blood cells (WBCs) often indicates a tubular disorder, whereas the coexistence with RBCs or WBCs could suggest glomerular issues. This specificity aids healthcare providers in tailoring appropriate treatment protocols and enhancing patient outcomes.
Can hyaline casts alone indicate kidney disease?
While the presence of hyaline casts is significant and can indicate renal stress, they alone are not sufficient to diagnose kidney disease. Additional diagnostic tests and clinical evaluations are necessary for accurate diagnosis.
How do hyaline casts differ from other types of casts?
Hyaline casts are smooth and translucent, whereas casts formed from white blood cells (WBC casts) are often more opaque and indicate inflammation. Red blood cell (RBC) casts suggest glomerular disease, while granular casts indicate more chronic or longstanding renal issues.
The presence of hyaline casts, though often benign, provides a pivotal clue in the intricate puzzle of renal diagnostics. By integrating routine microscopic examination of urine samples for casts, clinicians can proactively monitor kidney health and identify early signs of potential renal dysfunction. This proactive approach underscores the importance of comprehensive renal assessments, ensuring timely interventions and better patient care.