Sickle Cell Disease (SCD) is a significant public health challenge globally, especially within specific populations in Africa, the Middle East, and among Hispanic groups in the Americas. The condition, characterized by the abnormal shape of red blood cells, leads to severe pain episodes, organ damage, and a shortened lifespan. This article aims to provide an expert perspective on SCD, presenting practical insights, evidence-based statements, and actionable recommendations to enhance public health strategies.
Understanding Sickle Cell Disease
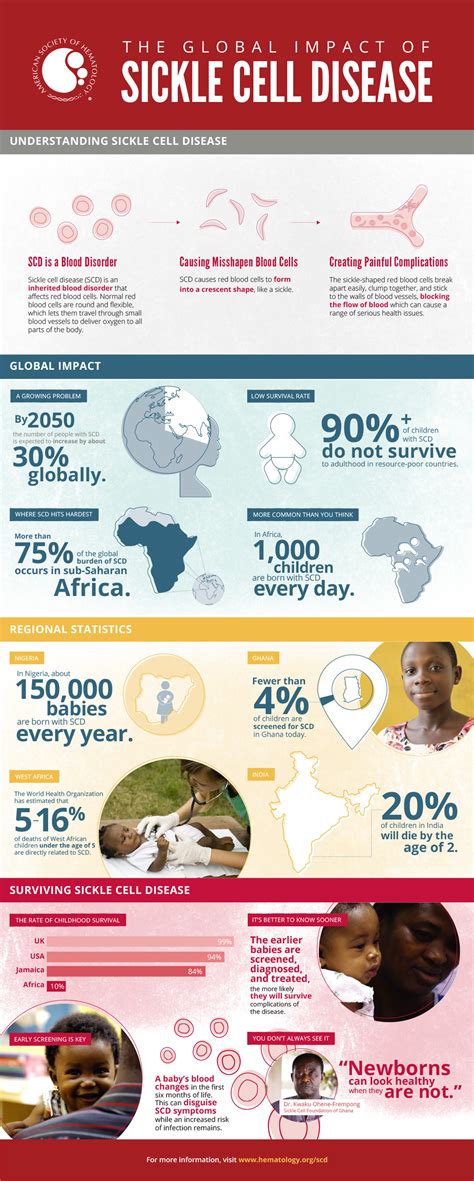
SCD affects millions worldwide, with approximately 300,000 babies born with the condition each year. The disease arises from a single genetic mutation that causes hemoglobin—a protein responsible for oxygen transport—to assume an abnormal form. This abnormality leads to red blood cells transforming into a sickle or crescent shape, which impairs their function and causes them to break down prematurely. The resultant blood cell rigidity also obstructs blood flow, leading to severe complications such as pain crises, infections, and organ failure.
Key Insights
Key Insights
- Early diagnosis and management are crucial to improving outcomes in SCD.
- Comprehensive healthcare strategies, including education and access to treatments, are essential to addressing the condition’s burden.
- Genetic counseling and screening programs can play a significant role in preventing new cases.
Clinical Management and Public Health Implications
The management of SCD involves a multifaceted approach addressing acute and chronic complications. Primary care providers must adopt a proactive stance to monitor patients for pain episodes, infections, and other acute issues. Evidence suggests that the use of hydroxyurea—a medication that increases fetal hemoglobin levels—can significantly reduce the frequency of pain crises and hospital admissions. Moreover, regular vaccinations and prophylactic antibiotics in early childhood help mitigate the high infection risk. Public health initiatives must, therefore, prioritize integrated care models that ensure continuous follow-ups and timely interventions.
Prevention and Genetic Counseling
Preventive measures are pivotal in managing SCD’s public health burden. The integration of newborn screening programs allows for early diagnosis and subsequent management strategies, which can drastically improve quality of life and life expectancy. Public health campaigns focused on education about SCD and genetic counseling can reduce the incidence of new cases. By offering genetic screening and counseling to at-risk couples, healthcare providers can empower individuals with knowledge, enabling them to make informed decisions regarding family planning. This approach not only benefits affected individuals but also reduces the societal and economic burden of the disease.
FAQ Section
What is the main cause of sickle cell disease?
Sickle Cell Disease is primarily caused by a genetic mutation in the hemoglobin gene, leading to the production of abnormal hemoglobin that distorts red blood cells.
How can public health programs support patients with SCD?
Public health programs can support SCD patients by providing access to comprehensive care, including early diagnosis, ongoing management, and preventive measures like vaccination and genetic counseling.
Sickle Cell Disease remains a formidable challenge in public health, necessitating coordinated, evidence-based efforts. Through early detection, integrated clinical care, and robust preventive programs, we can alleviate the disease’s burden and enhance the quality of life for those affected. The commitment to research, education, and policy development is imperative to advance our understanding and management of SCD, ultimately paving the way for a future with fewer individuals affected by this debilitating condition.