Navigating the road to recovery from bladder cancer can feel overwhelming, especially when trying to grasp the survival rates and prognosis. This guide aims to demystify these terms, offering clear, actionable advice that’s grounded in real-world examples. We’ll walk you through everything from understanding your diagnosis to post-treatment care, ensuring you have the practical tools to support your journey.
Bladder cancer is a significant health concern, affecting thousands annually. It's essential to understand that survival rates vary depending on several factors including the stage at diagnosis, type of treatment received, and individual health conditions. The aim of this guide is to provide a comprehensive overview, helping you feel more informed and empowered in your treatment decisions.
Understanding Bladder Cancer Survival Rates
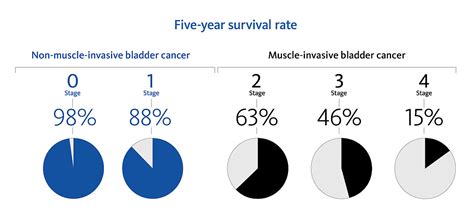
Survival rates are statistical tools that help healthcare providers and patients estimate the chances of recovery based on large groups of people with the same type and stage of cancer. For bladder cancer, these rates are often expressed as five-year survival rates, which measure the percentage of patients still alive five years after diagnosis.
Common Misconceptions
Many people misunderstand survival rates, believing they predict individual outcomes. It's important to remember that these are averages and don’t account for individual circumstances, treatments, and ongoing medical advances.
Quick Reference
- Immediate action item: Consult your oncologist for a detailed explanation of your specific survival rate.
- Essential tip: Stay updated with the latest research and treatments available for bladder cancer.
- Common mistake to avoid: Misinterpreting the five-year survival rate as your personal prognosis.
Early Detection and Diagnosis
Early detection of bladder cancer significantly improves survival rates. Recognizing symptoms early and seeking timely medical advice is crucial. Common symptoms include blood in urine, frequent urination, and pain during urination. If you experience any of these symptoms, it's important to schedule an appointment with your healthcare provider immediately.
Diagnostic procedures typically start with a physical examination and a urine test to check for blood. If these tests suggest bladder cancer, your doctor may recommend further imaging tests like CT scans or cystoscopy—a procedure where a thin, flexible tube with a camera is inserted into the bladder.
Quick Reference
- Immediate action item: Report any unusual urinary symptoms to your doctor.
- Essential tip: Ask your doctor about the various diagnostic tests available for bladder cancer.
- Common mistake to avoid: Delaying a medical consultation due to fear or misconception about bladder cancer.
Treatment Options
Treatment for bladder cancer often depends on the stage and type of the cancer. The main treatment options include surgery, chemotherapy, immunotherapy, and radiation therapy. Here, we'll go into detail about each option, including how they are used and their respective benefits and risks.
Surgical Options
Surgery is a common treatment for bladder cancer, especially for localized tumors. The two main surgical procedures are:
- Transurethral Resection of Bladder Tumor (TURBT): This procedure involves removing the tumor using a resectoscope inserted through the urethra. It's often used for early-stage cancers.
- Cystectomy: In this surgery, part or all of the bladder is removed. A partial cystectomy may be an option for some early-stage cancers, while a radical cystectomy is often needed for more advanced stages.
Recovery from surgery typically requires a hospital stay, and there can be complications such as bleeding, infection, or urinary incontinence. Following a specialized diet and physical therapy can aid in a smoother recovery.
Chemotherapy
Chemotherapy uses drugs to kill cancer cells or stop them from growing. It can be given before surgery (neoadjuvant) to shrink tumors or after surgery (adjuvant) to kill any remaining cancer cells. Chemotherapy can also be administered directly into the bladder (intravesical chemotherapy).
The benefits include reducing the risk of cancer recurrence and shrinking tumors. However, chemotherapy can cause side effects such as nausea, fatigue, hair loss, and potential damage to healthy cells.
Immunotherapy
Immunotherapy works by stimulating the body's immune system to fight cancer. Drugs like Bacillus Calmette-Guérin (BCG) and checkpoint inhibitors are used to treat bladder cancer. BCG is often used for non-invasive bladder cancer and can reduce the risk of cancer returning. Checkpoint inhibitors have shown promising results in treating advanced bladder cancers.
While immunotherapy can be highly effective, it’s important to be aware of potential side effects such as flu-like symptoms, skin rashes, and in rare cases, severe immune system issues.
Radiation Therapy
Radiation therapy uses high-energy rays to destroy cancer cells. It can be used alone for early-stage bladder cancer or in combination with surgery or chemotherapy for more advanced cases. The treatment typically involves daily sessions for several weeks.
The benefits include the possibility of removing the need for surgery and potentially curing the cancer. However, side effects can include fatigue, skin irritation, and in rare cases, damage to surrounding healthy tissue.
Quick Reference
- Immediate action item: Discuss all available treatment options with your oncologist.
- Essential tip: Prepare for side effects with your healthcare team to manage treatment outcomes better.
- Common mistake to avoid: Not considering all treatment modalities; surgery is not the only viable option.
Post-Treatment Care and Follow-Up
After completing treatment, ongoing care and follow-up are crucial for monitoring any signs of cancer recurrence. Regular follow-up appointments with your oncologist will include physical exams, urine tests, and imaging studies like CT scans.
Adopting a healthy lifestyle post-treatment can also significantly impact your long-term health. This includes maintaining a balanced diet, regular physical activity, and avoiding tobacco and excessive alcohol.
Regular follow-up appointments are essential for early detection of any signs of cancer recurrence. Your healthcare provider will advise on the frequency of these appointments based on your individual treatment plan and the stage of your cancer.
Quick Reference
- Immediate action item: Schedule regular follow-up appointments as recommended by your doctor.
- Essential tip: Maintain a healthy lifestyle to support your overall well-being.
- Common mistake to avoid: Overlooking follow-up care due to feelings of being cancer-free.
Frequently Asked Questions (FAQ)
What factors influence bladder cancer survival rates?
Several factors influence bladder cancer survival rates including the stage of cancer at diagnosis, the type and grade of cancer, the patient's overall health, and the type of treatment received. Early-stage cancers generally have higher survival rates compared to advanced stages. Additionally, personalized treatments and ongoing medical advancements can significantly impact survival rates.
Can lifestyle changes impact bladder cancer survival?
While lifestyle changes like maintaining a balanced diet, staying physically active, and avoiding tobacco and excessive alcohol can support overall health and well-being, they are not a direct influence on survival rates for bladder cancer. However, a healthy lifestyle can help manage side effects of treatment and improve the overall quality of life post-treatment.
What should I do if I notice blood in my urine?
Blood in urine, or hematuria, can be a symptom of bladder cancer but also other conditions. It’s crucial to consult your healthcare provider immediately if you notice blood in your urine. Early detection is key, so prompt medical evaluation can help determine the cause and appropriate treatment if necessary.